One of the distinguishing characteristics of living organisms is their capacity to move under their own power, i.e. to carry out motor behaviors. In a certain sense, all behaviors involve movement: whilst it is possible to separate out motion from other aspects of animal behavior, none of the behaviors crucial to sustaining life are possible without the ability to move from one place or position to another.
Motor capacity in humans can be affected by a broad range of debilitating disorders[1]. Investigating the causes and progression of motor disorders is vital for developing treatments, and mouse models are often used in this endeavor.
In this article, we will discuss a number of important tests used to assay motor capabilities in mouse models. The article will briefly explain how each test is used and what it is useful for, as well as discussing its upsides and downsides, and giving a few helpful tips to help researchers conduct experiments as smoothly as possible.
Motor Function and the Brain
In both humans and mice, several key regions of the brain are associated with motor behaviors. The motor cortex in the frontal lobe is believed to be responsible for controlling and initiating voluntary movements, such as lifting your arm or turning your head. The motor cortex is in turn divided into three sub-regions: the primary motor cortex, which generates most electrical signals intended to execute a movement; the premotor cortex, which prepares for and guides movements; and the supplementary motor area (SMA) which plans movements and coordinates the two halves of the body[2].
The cerebellum fine-tunes movements, but cannot initiate them. Its role is in adding guidance and precision to movements that are already occurring. It is also crucial for motor-related learning, and for maintaining posture[3].
The nigrostriatal pathway, which involves the substantia nigra and dorsal striatum, connects cognitive and motor functions. It is this pathway that is notably affected in Parkinson’s Disease[4].
The brain brings about voluntary movement via the spinal cord and peripheral nervous system, sending signals down to motor neurons which innervate muscle tissue and cause muscle contraction. Many forms of reflexive movement can occur via the spinal cord without the brain being involved. Furthermore, many repetitive motor behaviors, such as walking, can be maintained after initiation without further input from the brain by central pattern generators in the central nervous system.
Disorders Affecting Movement in Humans
Most human diseases affect movement capability to some extent, since energy and resources must be diverted to launching an immune and/or repair response. However, there are a number of conditions that are specifically associated with motor difficulties. These include neurological, skeletal, cardiovascular, and joint disorders.
Neurological Disorders
- Parkinson’s disease, in which loss of dopamine producing neurons in the substantia nigra reduces motor coordination and causes a distinctive “shakey” phenotype.
- Amyotrophic lateral sclerosis, also known as motor neuron disease, leads to the gradual loss of motor neurons and inability to achieve voluntary movement.
- Multiple sclerosis, which involves the degradation of the protective sheath around neurons, resulting in pain and difficulty walking.
- Huntington’s disease, where death follows rapidly after motor difficulties and cognitive decline.
Skeletal and Joint Disorders
- Osteoporosis, a broad disease category causing brittle bones and a stooped posture, making it difficult for the sufferer to bend over or reach up high.
- Sciatica, a spinal disorder resulting in severe back and leg pain and walking difficulties.
- Osteoarthritis and rheumatoid arthritis, the two major forms of arthritis, both cause swollen joints and severe pain when moving.
Cardiovascular Disorders
- Emphysema is a lung disease caused by loss of the small gas-exchanging sacks in the lungs; it leads to oxygen deprivation and fatigue, greatly reducing physical endurance.
- Asthma, an inflammatory disorder of the lungs, can also impact physical endurance since excessive exertion can provoke an attack.
- Heart disease can also decrease tissue oxygen perfusion and reduce endurance capability.
- Strokes, where blood flow is lost to a part of the brain, often cause paralysis on one side and subsequent difficulty coordinating movements.
Motor Tests
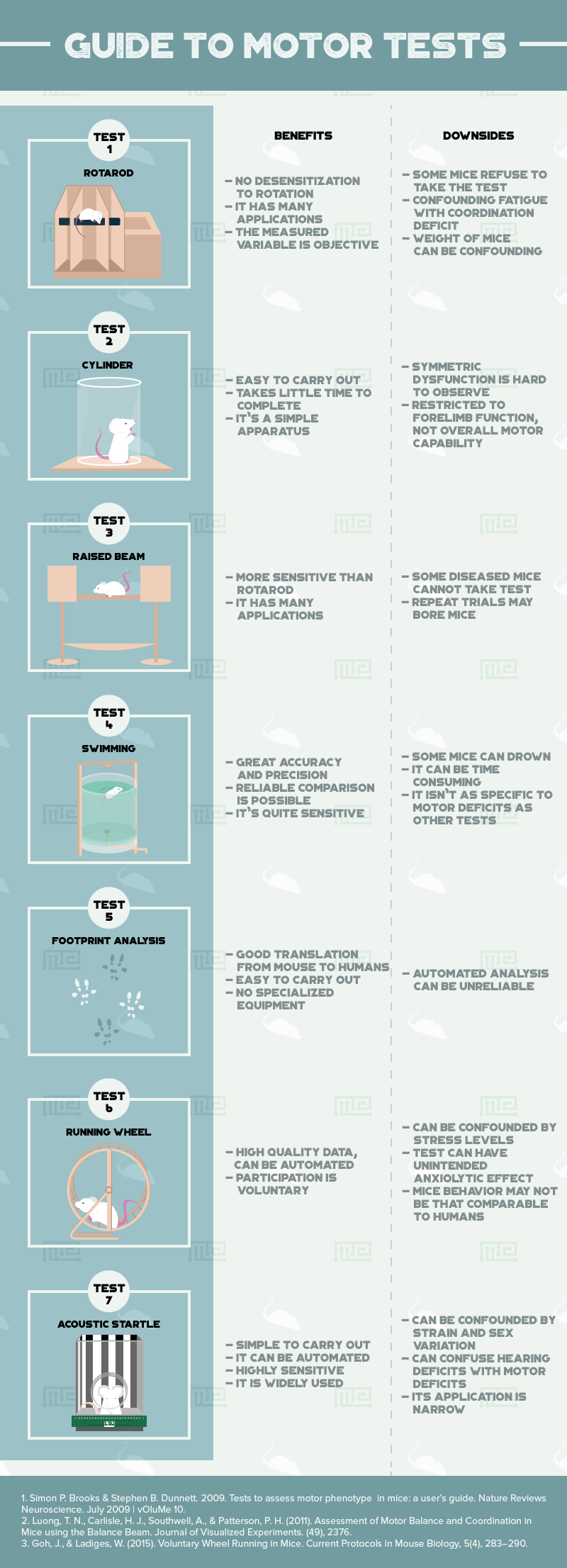
Now we will move on to discussing seven commonly used tests to assess movement in mice: the rotarod, cylinder, raised beam, forced swimming, footprint analysis, running wheel and acoustic startle.
Rotarod Test
The rotarod test is perhaps the most well known paradigm for assessing locomotor deficits in mouse models. The mice are placed onto a long, rotating rod and must constantly move forward and maintain their balance in order to avoid falling off. Sometimes the speed of the rotation is gradually increased throughout the trial. All mice have limited stamina and so will fall off the rod eventually, but mice with reduced motor coordination should remain on the rod for significantly less time than controls (or fall off at a lower speed).
Benefits
- Can re-trial, since individuals do not become desensitized to the rotation.[5]
- A wide array of different applications.
- Measured variable is objective, not confounded by subjective interpretation.
Things to Consider
- All mice must be placed on the rod with great care. If a mouse falls from the rod in under five seconds, it is likely the mouse was not placed properly, and so the experiment should be started again.
- The rod needs to have ridges on its surface to allow the mice to grip. However, having ridges which are too deep will allow the mice to simply hold on and travel with the rod rather than moving across it.
- Setting the initial speed too high will cause the results to be clustered at lower times, and so make it much harder to measure differences between the groups of mice.
Cylinder Test
The cylinder test was developed in the context of Parkinson’s Disease research,[6] and is specifically designed to investigate deficits in forelimb use. Each mouse is placed into a transparent, cylindrical enclosure, and then observed for a certain amount of time. Mice will naturally claw at the wall and attempt to escape. Comparing how much contact each mouse’s forelimbs make with the wall during the time period allows experimenters to see whether some of the mice have reduced forelimb function.
Benefits
- Inexpensive, simple apparatus.
- Test takes only a few minutes to complete.
- No complicated training required to carry out.
Downsides
- Symmetric forelimb dysfunction much harder to observe than asymmetric.[6]
- Restricted solely to forelimb function, not overall motor capability.
Things to Consider
- Ideally, the test should be done during the dark time of day when the mice are in the active part of their diurnal activity cycle.[7]
Raised Beam Test
Sense of balance in mouse models can be assessed with the raised beam test. Initially created to look at motor effects of ageing but also useful for assaying genetic models, this test requires the mice to walk across a narrow beam suspended above the ground, and reach a large platform on the other side. The time the mice take to cross the beam is recorded and compared, as is how many times they trip or slip. Mice with balance deficits will slip more often and take longer to cross.
Things to consider
- Sometimes the mice will remain stationary and refuse to cross to the platform. Giving the beam a positive gradient can encourage them to move forward, as mice like to run upwards.[6]
- Introducing the mice to the safe platform for a short while before running the test can increase their motivation to reach it.[6]
(Forced) Swimming Test
The forced swimming test is used as both a motor assay and an assay of mood (low performance is often considered indicative of depressive mood). The mice are placed into a tank of water and then swim around. Mice do not like water, and so will move around as much as they can to try and find a way to escape the tank. Sometimes a raised platform is included which the mice have to reach to get out of the water. Time to reach the platform can be measured, as well as swimming speed and limb movement. The test is most useful for investigating limb coordination.
Benefits
- Analyzing video of the trials provides great accuracy and precision.
- Common usage makes reliable comparison to previous results very easy.
- Decent level of sensitivity
Downsides
- Sometimes mice with especially severe motor deficits can drown.[6]
- Video analysis can be very time consuming.
- Not as specific to motor deficits as some other tests.
Things to Consider
- The water level should be marked on the tank to ensure it is the same for all trials.
- It can be useful to have a second water tank so that one tank can be prepared while the first is being used for an experiment, thus allowing faster transitions from one trial to the next.
- The depth of the tank should not be too shallow so the mice cannot touch the floor or climb out[9].
Footprint Analysis
This simple assay involves coating the feet of the mice in ink so that they will leave clear footprints when they move around. Different colors can be used on each foot. The footprints can then be analyzed to quantify various gait metrics such as stride length and width, and finger splay. This test has proven useful for Parkinson’s models[6].
Benefits
- Results translate very easily from mouse model to human.
- Easy to carry out.
- Does not require special equipment, unlike a treadmill test of gait.
Downsides
- Automated analysis has proven unreliable.
Things to Consider
- Make sure that the ink/dye used will not harm the mice or provoke any kind of allergic reaction.
Running Wheel
The running wheel is such a widely known apparatus for assaying mouse locomotion that it is even used outside of scientific experimentation. For largely unknown reasons, mice placed inside a rotating wheel powered by their own movement will continue to run on that wheel for extended periods of time. The test thus assesses voluntary movement: the mice do not even need to be placed in the wheel, as they will enter it of their own accord if it is placed in their enclosure. Distance travelled, average speed, time spent taking breaks, and various other dimensions can be recorded. The running wheel is a good test for general movement and motivation to move.
Benefits
- High quality data produced.
- Can be entirely automated.
- Mice voluntarily participates.
Things to Consider
- Mice of only one sex should be used in any one set of experiments, as the estrus cycle of the female mice affects their running behavior, and so will constitute a confounding variable if they are compared with males[6].
- The test should not be run for more than seven days at a time, to prevent long-term effects on the mouse phenotype[10].
- Mice should be acclimated to the wheel apparatus before the experiment starts to avoid evoking a novel object response[10].
Acoustic Startle
Both mice and humans exhibit a startle reflex when they suddenly encounter something unexpected in their environment. The response in mice is normally assessed by placing the mice inside a small chamber and then playing short, loud bursts of white noise at unpredictable intervals. The response can be removed by delivering a warning “pre-pulse”. The pre-pulse effect is often lost in disorders such as Huntington’s disease.
Benefits
- Simple protocol to carry out, and can be automated.
- High sensitivity and objectivity .
- Widely used, allowing easy comparison to prior results.
Downsides
- Can be confounded by differences in sex or strain.
- Can be hard to tease apart hearing deficits from CNS and motor deficits.
- Not especially broad paradigm, very narrow application.
Things to consider
- It is very important to first acclimatize the mice to the chamber before any sounds are played.
- A control with no sound stimulation must be included to allow for possible confounding variables such as weight to be identified[11].
Conclusion
Mouse models are extremely important in the scientific investigation of disorders affecting movement, and the development of effective treatment for those disorders. In order to obtain useful experimental results, it is crucial to choose the right protocol for each question, and to carry out that protocol as best as one can. Hopefully reading this article will have helped you to decide which motor tests will deliver the best results for your scientific endeavors.
For our apparatuses used in assessing rodent motor function see our Catalepsy bar test, Grip Strength test, the Balance Beam, the Parallel Bars, the Geotaxis Test, the Static Rods Test, the Gait Test, the Parallel Rod test, and the Pole test. See our activity range here.
References
- 2018. Movement disorders – Symptoms and causes – Mayo Clinic. [ONLINE] Available at: https://www.mayoclinic.org/diseases-conditions/movement-disorders/symptoms-causes/syc-20363893. [Accessed 05 June 2018].
- Cheney, PD. 1985. Role of cerebral cortex in voluntary movements. A review. Phys Ther. 1985 May;65(5):624-35
- Koziol LF1, Budding D, Andreasen N, D’Arrigo S, Bulgheroni S, Imamizu H, Ito M, Manto M, Marvel C, Parker K, Pezzulo G, Ramnani N, Riva D, Schmahmann J, Vandervert L, Yamazaki T. Consensus paper: the cerebellum’s role in movement and cognition. Cerebellum. 2014 Feb;13(1):151-77.
- William Dauer & Serge Przedborski. 2003. Parkinson’s Disease: Mechanisms and Models. Neuron. Volume 39, Issue 6, 11 September 2003, Pages 889-909.
- Cenci, Angela & Martin Lundblad. 2005. ‘Utility of 6-Hydroxydopamine Lesioned Rats in the Preclinical Screening of Novel Treatments for Parkinson Disease’ in Animal Models of Movement Disorders.
- Simon P. Brooks & Stephen B. Dunnett. 2009. Tests to assess motor phenotype in mice: a user’s guide. Nature Reviews Neuroscience. July 2009 | vOluMe 10.
- Fleming, S. M., Ekhator, O. R., & Ghisays, V. (2013). Assessment of Sensorimotor Function in Mouse Models of Parkinson’s Disease. Journal of Visualized Experiments. (76), 50303.
- Luong, T. N., Carlisle, H. J., Southwell, A., & Patterson, P. H. (2011). Assessment of Motor Balance and Coordination in Mice using the Balance Beam. Journal of Visualized Experiments. (49), 2376.
- Can, A., Dao, D. T., Arad, M., Terrillion, C. E., Piantadosi, S. C., & Gould, T. D. (2012). The Mouse Forced Swim Test. Journal of Visualized Experiments. (59), 3638.
- Goh, J., & Ladiges, W. (2015). Voluntary Wheel Running in Mice. Current Protocols in Mouse Biology, 5(4), 283–290.
- Acoustic Startle and Prepulse Inhibition. Dr. Maria Gulinello, Behavioral Core Facility, Albert Einstein College of Medicine, New York, USA. Accessed 3 June 2018. http://www.biobserve.com/behavioralresearch/wp-content/uploads/sites/2/2016/05/Acoustic-Startle-Protocol.pdf.